Alex Smith was 11 years old when he lost his right arm in 2003. A drunk driver operating a boat collided with his family’s vessel on Lake Austin, sending him overboard. He hit a propeller, and his arm was severed in the water.
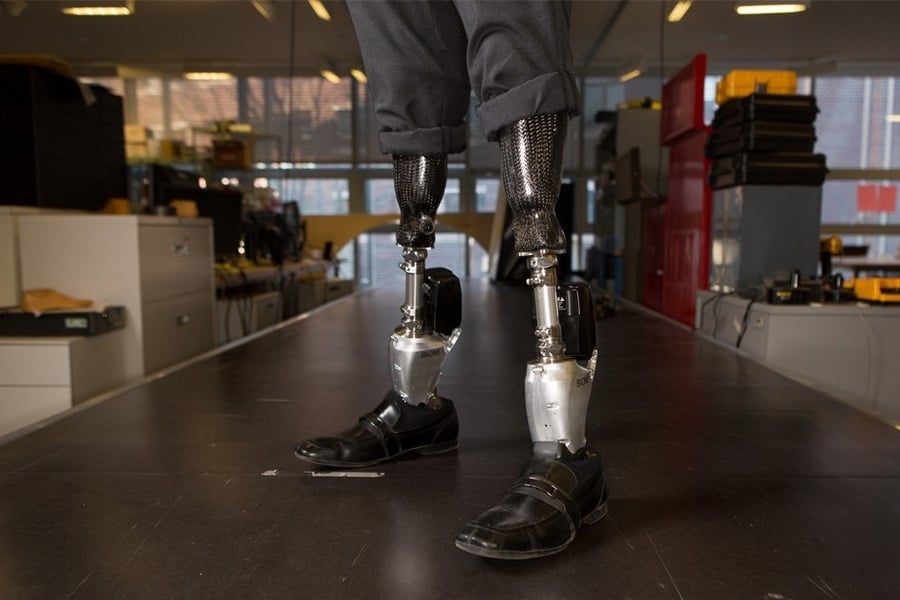
A year later, he got a myoelectric arm, a type of prosthetic powered by the electrical signals in his residual limb’s muscles. But Smith hardly used it because it was “very, very slow” and had a limited range of movements. He could open and close the hand, but not do much else. He tried other robotic arms over the years, but they had similar problems.
“They’re just not super functional,” he says. “There’s a massive delay between executing a function and then having the prosthetic actually do it. In my day-to-day life, it just became faster to figure out other ways to do things.”
Recently, he’s been trying out a new system by Austin-based startup Phantom Neuro that has the potential to provide more lifelike control of prosthetic limbs. The company is building a thin, flexible muscle implant to allow amputees a wider, more natural range of movement just by thinking about the gestures they want to make.
“Not many people use robotic limbs, and that’s largely due to how horrible the control system is,” says Connor Glass, CEO and cofounder of Phantom Neuro.
In data shared exclusively with WIRED, 10 participants in a study conducted by Phantom used a wearable version of the company’s sensors to control a robotic arm already on the market, achieving an average accuracy of 93.8 percent across 11 hand and wrist gestures. Smith was one of the participants, while the other nine were able-bodied volunteers, which is common in early studies of prosthetics. The success of this study paves the way for testing Phantom’s implantable sensors in the future.
Current myoelectric prosthetics, like the ones Smith has tried, read electrical impulses from surface electrodes that sit on the amputated stump. Most robotic prostheses have two electrodes, or recording channels. When a person flexes their hand, their arm muscles contract. Those muscle contractions still occur in an upper limb amputee when they flex. The electrodes pick up electrical signals from those contractions, interpret them, and initiate movements in the prosthetic. But surface electrodes don’t always capture stable signals because they can slip and move around, which decreases their accuracy in a real-world environment.
Existing devices also have a limited range of gestures, and to control those gestures, prosthetics wearers must make movements that usually do not correlate to the gesture they want to make. For instance, they may have to flex their wrist down to carry out a pinching motion. Alex’s current prosthetic has the capability to perform around 20 gestures, but he can only program four of them onto the device at a time. He has to toggle between those different hand functions sequentially, which means moving from gesture A to gesture B and so forth. In other words, he can’t jump from gesture A to gesture D.
In a 2020 survey of upper limb amputees, 20.7 percent used myoelectric prostheses while 74.4 percent used body-powered prostheses—devices with hooks that can open and close, operated by body movement and a pulley system. There were no differences in user satisfaction between prosthesis types, and of those who reported using myoelectric prostheses, 44 percent went on to abandon them altogether.
Phantom is aiming to interface directly with the muscles to give users more natural control, but the company had to test a wearable version of its muscle sensor before it can implant the device in volunteers. While the wearable version performed well, Glass says it’s not ideal for everyday use. Like existing prosthetics, it can slip and move around, which affects its accuracy. Because of this, wearables have to be recalibrated often. He says an implant will be more reliable, and may be able to achieve even higher accuracy since it won’t have to read electrical signals through the skin. Glass envisions that the implantable version will be inserted through a small incision and fed under the skin.
“We’re picking up the electrical activity directly from the surface of the muscle,” he explains. Movement intention originates in the brain, which sends electrical impulses through the peripheral nerves to tell the muscle to contract. In amputees, those neural pathways are still intact.
For the wearable study, Smith and the other study participants had an hourlong training session to get introduced to the technology and came back on a second day to perform the trial. After a 10-minute algorithm-calibration process on the trial day, participants were instructed to make 11 gestures—including open hand, close fist, pinch, thumbs up, index point, index finger click, rotate wrist in, and rotate wrist out—multiple times each while Phantom’s software learned and decoded their muscle signals into those actual movements. For the able-bodied participants, it meant that a robotic arm was mimicking their gestures. For Smith, the prosthetic made the movements he was simply thinking of making. “It was the coolest experience,” he says.
Participants wore two thin sensors, each with 16 electrodes. Gesture decoding accuracy ranged from 84.8 percent to 98.4 percent in the participants, with a latency—the time it takes from signal detection to gesture execution—of less than 200 milliseconds. A natural human latency, the delay between neural signals arriving at the muscle and the muscle actually executing that movement, is roughly 100 milliseconds.
“The rapidity of their ability to get those classification accuracies is huge,” says Paul Marasco, a neuroscientist at the Cleveland Clinic, who studies natural touch and movement for artificial limbs and isn’t involved with Phantom. “The faster that you can do that, the better off you are, and the more seamless the system can get.”
Some companies are developing brain implants that would allow paralyzed people to control prosthetic limbs with their thoughts. Those systems, known as brain-computer interfaces, read and decode signals in the brain to allow the prosthetic to carry out intended movement. Elon Musk’s startup Neuralink announced last month that it is launching a study to test whether its brain implant can allow participants to directly control a robotic arm.
Geoffrey Ling, a technical adviser to Phantom and the founding director of the Biological Technologies Office at the US Defense Advanced Research Projects Agency, says brain implants carry more risks and need to be very long-lasting so that patients don’t have to undergo multiple brain surgeries. “The peripheral nerves are a very attractive approach because it’s minimally invasive,” he says. Phantom believes its implant could be inserted during an outpatient procedure without the need for a specialized surgeon.
Phantom plans to begin a clinical trial for its implanted version, which will enroll upper limb amputees, in 2025. Smith hopes to be involved in that study. If the Phantom technology makes it to market, he could see it helping amputees like him be able to do everyday tasks more easily. “I think this is going to be a total game changer.”
Emily Mullin is a staff writer at WIRED, covering biotechnology. Previously, she was an MIT Knight Science Journalism project fellow and a staff writer covering biotechnology at Medium's OneZero. Before that, she served as an associate editor at MIT Technology Review, where she wrote about biomedicine. Her stories have also... Read more